REPRODUCTIVE, MATERNAL, NEWBORN, CHILD AND ADOLESCENT HEALTH
REPRODUCTIVE, MATERNAL, NEWBORN, CHILD AND ADOLESCENT HEALTH
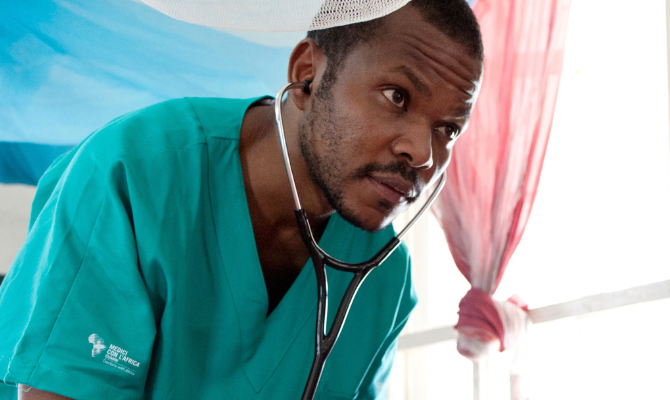
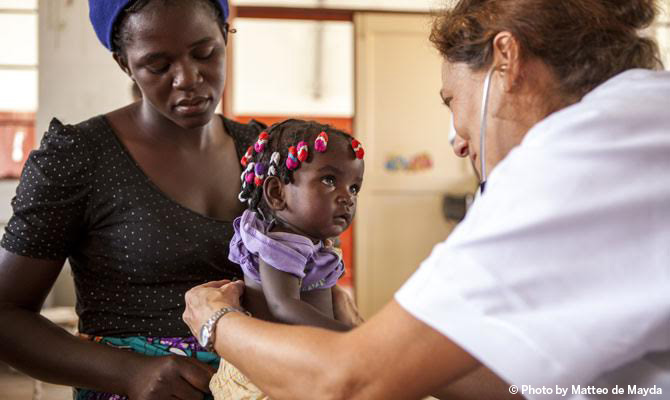
Maternal, neonatal, child, and adolescent health represent crucial public health challenges in sub-Saharan Africa. They are among the primary health objectives in the new Sustainable Development Goals and they represent a priority for Doctors with Africa CUAMM. Points of particular concern are the serious issue of inadequate progress in reducing neonatal mortality, high mortality from diarrhea and lung infections for children under 5 years old, adolescent pregnancy, maternal mortality and violence against women in all its forms. Maternal mortality and access to services for reproductive health and obstetric emergencies are among the key indicators of the level of social inequality between developed and less developed countries and between rich and poor people within a country. Indeed, access to quality maternal care services is a proxy of the status of a health system as a whole. It shows the existence of basic and advanced quality obstetric services in operation at all times of day and a consistent availability of a qualified workforce, medicine and equipment (including the option of blood transfusions), transportation and communications that connect families and communities with the peripheral health network and hospitals, following a continuum of care approach.
NUTRITION
A major priority in the Sustainable Development Agenda and for Doctors with Africa CUAMM is increasing the focus of ensuring good nutrition during pregnancy and in early childhood. Recent financial and food crises have negatively affected access to food, especially by the poorest parts of the population. The effects of malnutrition on fetuses, infants, and children are well-known and include reduced fetal growth; increase susceptibility to infectious diseases in early life and chronic diseases in later life; and impaired physical and cognitive development in the medium- to long-term. Acute malnutrition (“wasting,” low weight for height) is due to acute shortage of food or diseases and it poses a high risk of death for the child. Many countries in sub-Saharan Africa have a prevalence adolescence of wasting over the threshold of 5% and up to over 20% (such as South Sudan). The prevalence of chronic childhood malnutrition (“stunting,” low height for age) is caused by poor or insufficient diets, poor levels of care for a child and the coexistence of diseases. It affects mainly poor populations and families. The prevalence of chronic malnutrition in sub-Saharan Africa has declined only a few percentage points from 1990 to 2010; in some cases, it is found in over 30% of the pediatric population. A 40% reduction target has been set for 2025.
INFECTIOUS DISEASES
Despite progresses, much of the African population continues to suffer from preventable premature death and disability caused by major epidemic diseases. Doctors with Africa CUAMM works to fight Malaria, HIV, Tuberculosis and neglected tropical diseases. These diseases, also known as “infectious diseases of poverty” affect especially the most vulnerable and poor who live in rural areas and urban slums where it is difficult to access, use, and adhere to prevention, treatment and follow-up. Those at greater risk are pregnant women, children, adolescents and adults living in disadvantaged social conditions. Effective responses to new, ambitious, international targets to fight infectious diseases should combine major investment in research, development and delivery of new drugs and vaccines together with mobilization of resources for overall health system strengthening. A far as the latter is concerned, Doctors with Africa CUAMM works to improve integration of disease treatments (e.i. co-management of HIV and TB patients), levels of care (hospital, health centres and communities) and human resources (qualified health personnel and community health workers).
NONCOMMUNICABLE DISEASES AND TRAUMAS
Aging processes, urbanization, economic development and the spread of risk factors in Africa are at the root of the dramatic rise in chronic diseases and traumas, especially in urban areas. The impact of Noncommunicable diseases and traumas in terms of premature death and disability join those of maternal and childhood diseases and infectious diseases (“double burden”). The problem is profoundly complex. Chronic patients are usually affected by more than one disease (multimorbidity), including infectious diseases, such as HIV/AIDS. This exposes them to serious, prolonged social and economic consequences, including bearing catastrophic healthcare costs. This form of “hidden inequality” is exasperated by fragmented patient management that follows a care model more focused on individual diseases than on people, difficulty in accessing basic diagnostic tests, essential medicine, competent medical personnel, and the basic lack of any form of protection from financial healthcare risk. In order to respond more effectively, equitably, and sustainably to chronic diseases, we need multisector fiscal policies, integrated prevention programs, psychological and pharmacological intervention packages of proven efficacy, systems for recording vital data, monitoring and surveillance of individual and population risks, and innovative forms of integration and synergy with other health programs. Innovations also need to be made in the relationships between patients and health workers. Patients suffering from chronic diseases, if empowered by trained health workers, can learn over time to be skilled in self-managing risk factors, episodes of illness, and multi-morbidity.